It is clear that medication adherence is a challenge for the healthcare ecosystem. Deploying a multimodal approach whereby interventions including patient education, packaged medications, and a pharmacist calling patients in order to stay connected have produced success. However, implementing this complex combination in part or in totality is resource intensive, financially unsustainable and quite frankly not feasible in a pharmacy environment.
Pharmacy wants and needs medication adherence for very important reasons:
1. More fill and refills drives top line revenue.
2. Adherence to medication therapy maximizes the pharmacy’s opportunity to drive 5 star ratings.
3. Allows participation in narrow networks.
4. Preservation of payer driven revenue that is always at risk for poor performance.
Pharmacy has historically embraced technology and it could be argued, has been an early adopter of scalable automation manifested in interventions such as automated order ready, vaccination reminders and real time POS billing.
For pharmacy to create the proverbial “paradigm shift” in medication adherence, a technological approach is needed that is patient centric, personal, driven at the medication or therapeutic class level, which also can empower the pharmacist as a provider.
Communication interventions with texting and secure messaging can be designed to keep the patient connected through their acute or chronic course of therapy that is driven by patient preference, constructed with content from pharmacists’ knowledge, sequenced based on drug nuance and can be conversational in nature. This done at scale is where pharmacy and technology need to dance.
The pharmacy imperative is to springboard from the use of scalable automation to drive basic business success to leveraging technology in such a fashion that the vision of pharmacist and pharmacy as an empowered provider comes to fruition.
Digital Conversation is in a unique position to act upon this imperative based on the current role we play, the assets that we have, and our unique acumen in communication.
Digital Conversation will drive refill reminders with SecureRx©, create scalable outreach with Campaigns, clinically engage the patient with Pathways©, allow the patient to initiate digital messaging with Enhanced Chat© and deliver a host of secure web-based applications to improve workflows and maximize a pharmacy’s resources. In addition Digital Conversation can control the content, frequency and sequencing of that messaging based on the data we receive from the pharmacy. By elevating the messaging to a personal approach driven by an understanding of who the patient is and what medications are taken is an opportunity for DC to increase revenue and create a digital ecosystem for pharmacy.
What we want to do is receive a data payload and include elements that would allow us to understand more about the patient and their therapy, whereby allowing us to participate in the content, frequency and sequencing of the messaging, creating a more connected patient, and maximizing medication adherence.
What do we need to do?
There are both tactical steps that need to be initiated and philosophical edicts to overcome. The first philosophical edict must be a recognition that DC needs to hold data and use that data, with permission from our clients, to maximize messaging and outcomes for the patient. The first tactical step is to recognize that the payload must expand.
What is the Data from pharmacy and what does it mean?
Generally speaking, pharmacy data can be organized into the following domains:
- Patient
- Product
- Prescription
- Plan
- Prescriber
These domains are affectionately called the five “P”s.
PATIENT
This is typically patient demographic data that reflects elements such as name, address, city, state, zip code, cell phone number, home phone number, birthdate and gender. Some additive elements that help process a prescription often times includes drug plan indicator, relationship to card holder of drug plan, expiration date.
PRODUCT
This is the medication that is dispensed to the patient. The medication is coded within a claim with the National Drug Code. The National Drug Code is a unique 10-digit, 3-segment numeric identifier assigned to each medication listed under Section 510 of the US Federal Food, Drug, and Cosmetic Act. The segments identify the labeler or vendor, product (within the scope of the labeler), and trade package (of this product).
• The first segment, the labeler code, is 4 or 5 digits long and assigned by the Food and Drug Administration (FDA) upon submission of a Labeler Code Request. A labeler is any firm that manufactures, repacks or distributes a drug product.
• The second segment, the product code, is 3 or 4 digits long and identifies a specific strength, dosage form, and formulation for a particular firm.
• The third segment, the package code, is 1 or 2 digits long and identifies package forms and sizes. In very exceptional cases, product and package segments may have contained characters other than digits. [2]
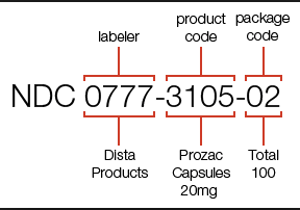
By adding NDC to our data payload, a sampling of what we would now know from the prescription, about the patient and the drug therapy would be the following:
1. What the drug is.
2. What the drug is used for
3. How the drug is given
4. The price of the drug
5. The side effects of the drug
6. The route of an administration
7. What disease the patient is being treated for
8. If there are contraindications for the drug
9. How frequent this particular drug is dispensed
10. If this drug represents that most revenue in a campaign
11. What drug company manufacturers this product.
PRESCRIPTION
These are the details of the transaction. The elements that make up the prescription provide context to the therapy of the patient. Prescription or RX number is a number assigned by the pharmacy that is unique to their software application. The prescription numbers is what patients “call in” to get refilled. The quantity represents how much of the drug was dispensed. This numeric value references number of pills, how much liquid (milliliters), or how much cream or ointment (milligrams or grams). The days of supply is an input number from the pharmacist representing how many days the supply of medication will last. As an example, if an antibiotic is dispensed as 28 tablets, with one tablet taken 4 times per day, then the days of supply are 7. The date the prescription was filled, the date the prescription was ready, the date the prescription was picked up, the date the prescription is due for a refill. This last date is often calculated based on original date filled and then adding the number from the days of supply to calculate when the next refill of that prescription is due. The prescription also holds the name of the medication, national drug code, patient name, doctors name, prescription plan, additional patient identification numbers unique to the plan they are on, and additional information that may be unique to the pharmacy’s practice.
PLAN
This information designates who and under what type of insurance plan the prescription medication is covered. A third party pays for over 70% of all prescriptions with some patient liability. Many times in addition to identifying the plan, information is also held on how to send a prescription claim electronically. The plan is usually assigned a processor control number and BIN number for routing of a claim electronically to a fiduciary intermediary.
PRESCRIBER
This is the physician information. It includes basic demographics such as address and phone numbers and in addition Prescriber Identification Numbers. This is either a NPI number, tax identification number or in rare cases a social security number.
What does Nirvana look like? Pharmacy data is sent to Digital Conversation which includes every transaction from their system that is subject to a refill reminder. We build a database unique to that customer that allows us to maximize the multiple text delivery methodologies we offer and provide a prescriptive state of communications for their patients such that an exceptional, un-parallel engagement experience is provided.
1. We receive a payload from an API.
2. We ingest the data payload and apply business processes.
3. We execute on our SecureRx© messaging for Refill Reminder without the need for a mobile App.
4. We then assign Pathways© to those patients that we have identified as non-adherent. We maximize medication adherence prospectively not retroactively as is done today. The need for organizations like Outcomes MTM goes away. Payers see the value of identifying non-adherence up front and engaging the patients at the time of dispensing and throughout the course of therapy. Text messaging changes behavior to the positive.
5. Our client supplements SecureRx© campaigns and Pathways© with a DC Enhanced Chat© and Campaign functions that allows for the conversation to be sustained at scale.
6. The messaging now morphs from basic blocking and tackling to a personalized message curriculum that creates an electronic conversation.
7. The pharmacist now has created a digital conversation at scale that is more intimate and detailed (yet requires less work, resource and time), and through Pathways©, captures how the patient is feeling, if they have taken all their meds, reminds them of the number of pills they should have left, links to a video, provides patient education. All done at scale through empathetic automation.
8. The database has been built over a year; the client says they want to do a specific Campaign around their diabetic patients.
9. We run a query and find all the eligible diabetics because we know their drug therapy.
10. We craft a pathway that maximizes market basket and therapeutic management of the patient. Top line revenue improves. Additional campaigns are identified and crafted.
“I want to put a ding in the universe.” — Steve Jobs






